Traditional Thai Massage for Short-Term Back Pain Management
Traditional Thai massage, or TTM, is part of traditional Thai medicine. This massage includes deep pressure massage with sustained compression on a muscle. Passive stretching is included at the completion of the massage. Previous research on TTM has found a variety of benefits, ranging from increased flexibility and decreased muscle tension, to reduced pain. The traditional massage is guided by lines on the body, called the Sen Sib. These imaginary lines serve as directions for the massage therapist, who applies pressure to points across these lines. The Sen Sib, however, falls on most of the trigger points on the body, which may explain its effectiveness.
Researchers Buttagat, Narktro, Onsrira, and Pobsamai (2016) wanted to look into the effectiveness of TTM, specifically concerning myofascial pain syndrome. Myofascial pain syndrome (MPS) is not an uncommon condition. It is characterized by localized pain and may include a decrease in range of motion, problems with sleep, and the presence of myofascial trigger points. Skootsky, Jaeger, & Oye (1989) found that MPS occurs most often in the upper body, and Rachlin and Rachlin (2002) elaborated further, explaining that the most common areas affected are in this order: the trapezius, levator scapulae, and axial postural muscles.
While previous research has looked into the effectiveness of TTM on myofascial pain syndrome, the researchers felt like there needed to be more concrete evidence on its efficiency. For their 2016 study, they used electromyography (measurement of muscle energy) to measure the effect of TTM on muscles.
The researchers conducted a single-blind, randomized clinical trial consisting of 50 participants. These participants had to have suffered from upper back pain for at least three months prior to the study, with the presence of at least one myofascial trigger point in the upper trapezius muscles. The researchers noted that, “the criteria used to diagnose MTrP described previously by Buttagat et al. (2016) was as follows; the presence of a tender nodule that causes a referred pain within taut bands of muscle in areas which the patient identified as painful.”
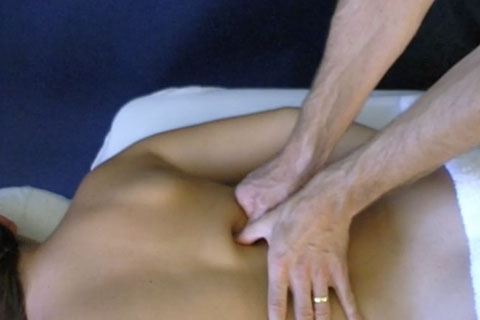
The 50 participants were randomly assigned to one of two groups, TTM or control. For the TTM group, participants lay down on their side while fully clothed. For 30 minutes, the massage therapist used the thumb or another digit to apply body weight onto different points of the upper back, slowly increasing pressure for a duration of 5 to 10 seconds per point. At the end of the massage, the massage therapist would passively stretch the participants’ muscles. The control group did not receive any actual treatment. The researchers set up a micro-wave therapy machine next to the participant. The machine was turned on, but was kept in standby mode as a form of placebo therapy. This intervention also lasted for 30 minutes.
The researchers measured EMG activity as well as participants’ ratings of perceived muscle tension and pain intensity. These variables were measured both before and after intervention.
Participants in the TTM group showed a significant decrease in all three variables – EMG activity decreased, as did reported muscle tension and pain intensity. The control group had almost no change to EMG activity or reported pain, but the control group participants did surprisingly report a decrease in muscle tension.
Traditional Thai massage seems to provide beneficial results for patients with upper back myofascial pain syndrome. These results support the findings of existing research on the benefits of TTM. The researchers indicate that long-term studies on the effect of TTM would be ideal, but that based upon the results of the study, TTM is “a useful intervention for promoting physical relaxation and decreasing muscle tension and pain in MPS patients.”
References
Buttagat, V., Narktro, T., Onsrira, K., & Pobsamai, C. (2016). Short-term effects of traditional Thai massage on electromyogram, muscle tension and pain among patients with upper back pain associated with myofascial trigger points. Complementary Therapies in Medicine, 28, 8-12. doi:10.1016/j.ctim.2016.07.004
Buttagat, V., Taepa, N., Suwannived, N., & Rattanachan, N. (2016). Effects of scapular stabilization exercise on pain related parameters in patients with scapulocostal syndrome: A randomized controlled trial. Journal of Bodywork and Movement Therapies, 20(1), 115-122. doi:10.1016/j.jbmt.2015.07.036
Rachlin, E., & Rachlin, I. (2002). Chapter 11 – Trigger Point Management. In Myofascial Pain and Fibromyalgia (2nd ed., pp. 231-258). St. Louis, MO: Mosby.
Skootsky, S., Jaeger, B., & Oye, R. (1989). Prevalence of myofascial pain in general internal medicine practice. Western Journal Of Medicine, 151(2), 157-160.






Follow Us!